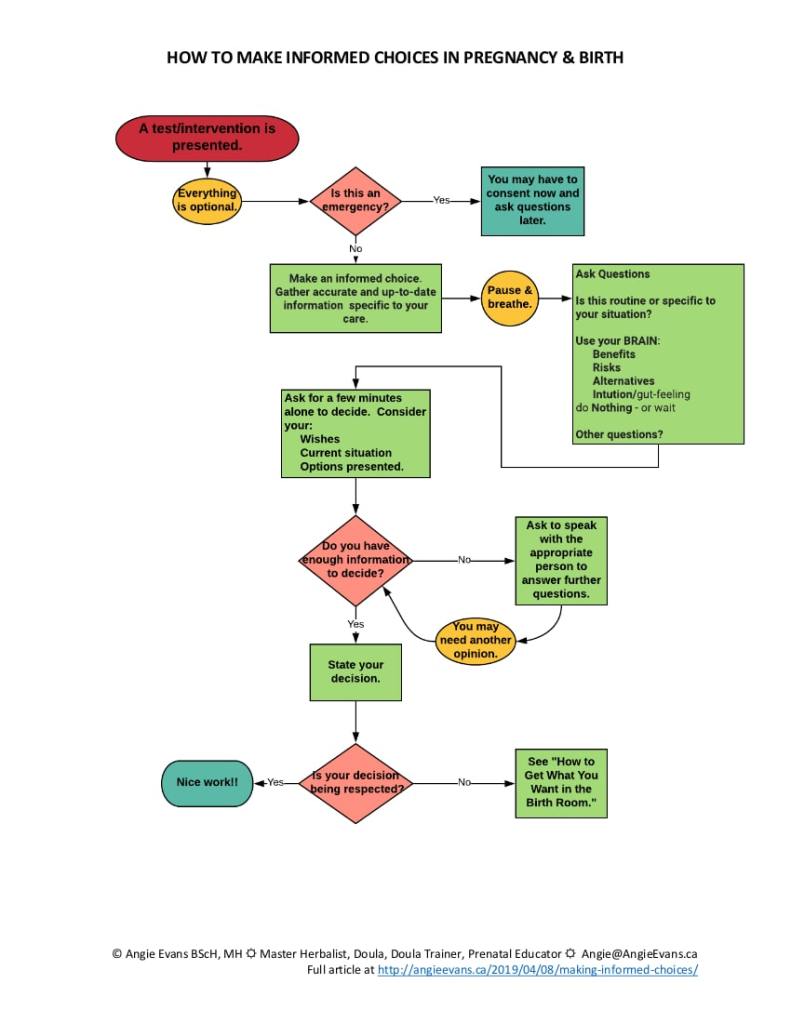
You know informed choice is a legal right but how do you make those choices? Here’s some guidance to help you get information and ask questions, so you can be an active participant in your health care.
While tests and interventions may not be introduced in a way that implies they’re optional, they are. Everything is optional. In my experience personally and as a birth attendant, medical staff are patient, respectful and happy to answer questions when asked.

Lots of folks ask how they’ll know if something’s urgent or an emergency. Immediate urgent situations are far less common than people think. In real life, the sudden and severe catastrophes depicted in mainstream media are uncommon.
Normally a healthy pregnancy is followed by healthy labour and birth. Most problems come with warning signs that medical professionals see developing. They do their best to monitor and address those situations well before emergencies arise. If there’s actually no time for discussion then your medical care provider will tell you that, and then answer your questions later.
If everything is optional and a choice, then how do you decide? You need to gather accurate and up-to-date information that’s specific to your care.
- Policies and practises change over time.
- Public health policies are created for the entire population, not for you specifically.
- “Dr. Google” is scary.
- People often share scary stories or inaccurate info (even though everyone talks like an expert).
Keep an open mind and make the best decisions you can at the time, with the given circumstances and information available.
Preparation!!
Learn options through wise counsel, before your labour begins.
- Ask people (who are giving birth in the same area as you) what they liked and didn’t like about their experience. Note these people likely don’t know all the options that are actually available.
- Ask a professional who currently works in obstetrics in your area what the regular practises and routine procedures are. (RNs, your MW/MD/OB, your doula.)
- Seek information that’s presented thoughtfully and respectfully. Be wary of extremes such as, “Just trust birth and don’t let anyone touch you” or the opposite, “I’m the captain of this ship and I’ll tell you what to do.”
- Create a birth-plan or list of preferences that builds bridges with your care team.

In the Birth Room:
When a test or intervention is being recommended (which is often not presented as a choice or recommendations, but rather a “have to”):
- Remember everything is a choice / everything is optional.
- Push the PAUSE button and ask questions.
- You can use the BRAINS acronym (Benefits, Risks, Alternatives, Intuition / gut-feeling, do Nothing or wait longer, Sign the waiver).
- If that’s too much, simply tell everyone to pause and then ask, “What’s happening?” or “Why is this being recommended?”
- Always consider the health of the maternal patient and the baby in this moment. Your medical team can make you aware of trends that concern or reassure them.
- Ask about timelines. What if you wait a few minutes, an hour, several hours or days? Note – this will vary with birth-places and depend on things like if you need to be transferred to another location, if medical personnel have to be called in or if everyone and everything needed is already available, how busy the unit is.
- If you don’t understand the words being used, ask for clarity. Sometimes people at work forget that not everyone speaks the same technical language.
Take some time.
- State that you’d like a few minutes alone to decide.
- Consider the information that was presented and check in with your gut-feelings. Admittedly it’s hard to discern between intuition and fear during labour and when your baby is involved.
- If you need more information, then ask the most appropriate person.
- Consider a second opinion. Often you’ll get different answers from different professionals.
- Do you have further questions or need more info?
State your decision. If your choice isn’t being respected then see “Getting What You Want in the Birth Room.”
Here’s a printable pdf of the graphic: How to Make Informed Decisions in Pregnancy & Birth.